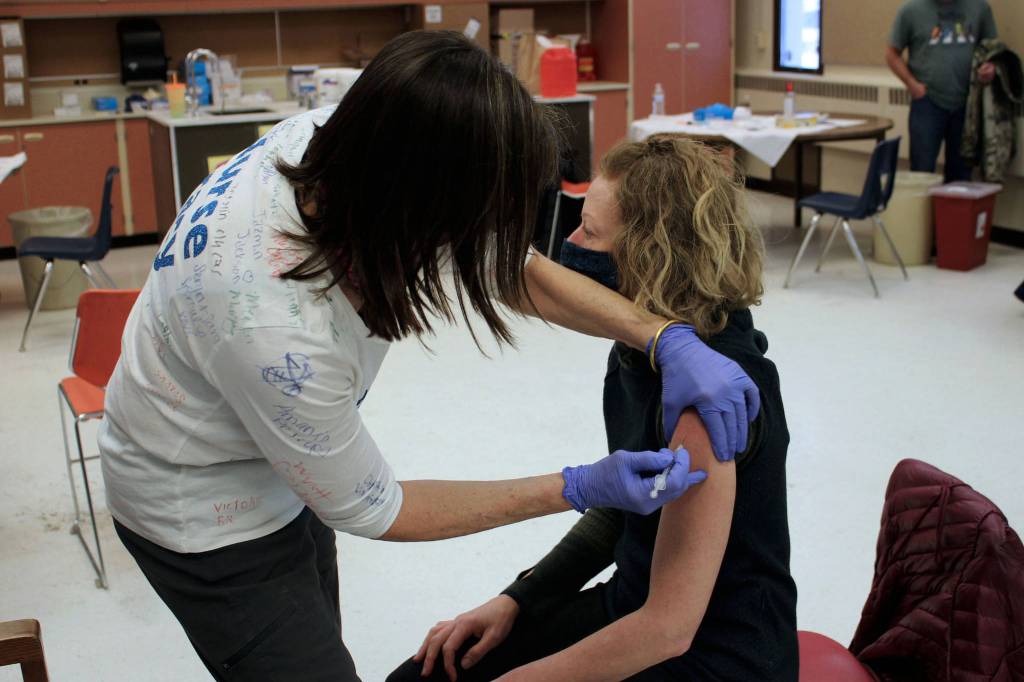
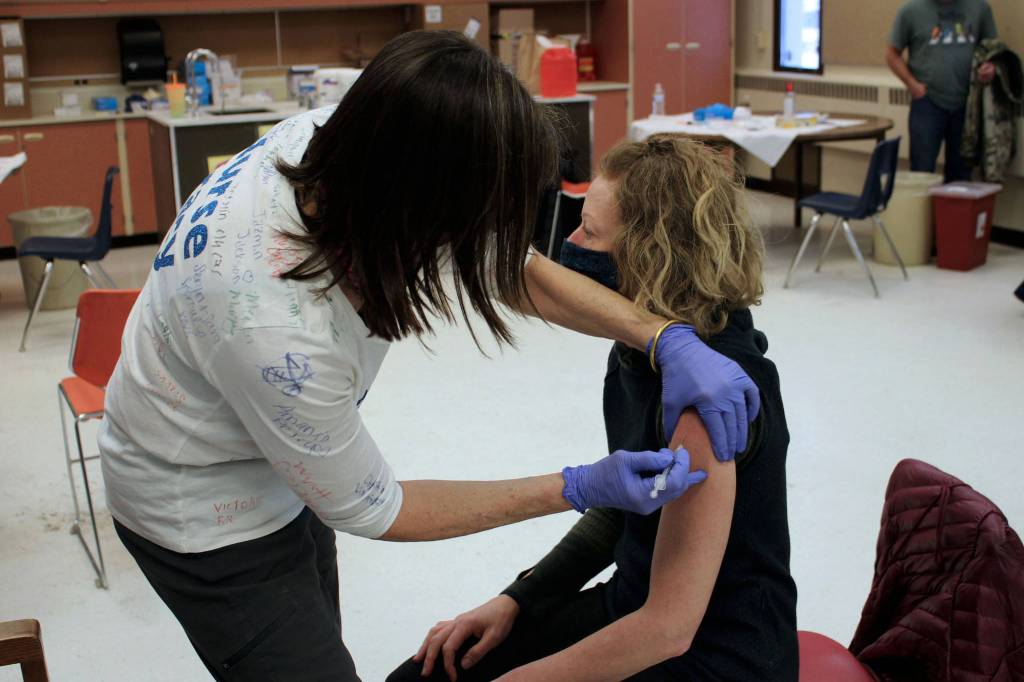
‘Get the vaccine’
Published 10:30 pm Tuesday, April 6, 2021


Lingering effects of COVID-19 have raised concerns among health officials, but they say the best way to prevent “long COVID” — or the persistence of COVID-19 symptoms for weeks after their initial onset — is to not get COVID at all.
That means following mitigation strategies that have been shown to stop the spread of COVID-19, such as wearing a mask and social distancing, and to get vaccinated against the virus, according to Kenai Public Health Nurse Manager Leslie Felts.
“Wear masks, wash hands, keep cohorts small, keep a distance from others to avoid respiratory transmission of COVID-19,” Felts said.
Felts said that there is no universal definition of long COVID and that rather it is a “catchall” phrase used to describe COVID-19 symptoms that last more than a few weeks after the initial onset of COVID symptoms. Those symptoms can vary widely, but include shortness of breath, brain fog, fatigue, headaches, dizziness and anxiety or depression, among others. Felts said long COVID is being studied by scientists as “Post-Acute Sequelae of SARS-CoV-2,” or PASC.
That lack of a universal definition of the condition means any tracking efforts rely on the individuals who choose to self-report their symptoms, Felts said.
“Just like this whole pandemic has been an ongoing learning (process), trying to determine what course this virus is going to take, how it’s going to affect people, and then trying to come up with the best solutions, it’s just an ongoing process,” Felts said.
Public health officials with the Alaska Department of Health and Social Services have said that the issue of long COVID is “definitely concerning,” but also emphasized that the best way for people to avoid developing long-term COVID symptoms is to not get COVID at all.
“If you’re vaccinated you’ve got a high chance of not getting COVID and if you don’t get COVID you’re not going to get long COVID,” State Epidemiologist Joe McLaughlin said during a press briefing in late March.
McLaughlin noted a research letter published in the Journal of the American Medical Association, a peer-reviewed medical journal, last year. The study surveyed 143 COVID-19 patients in Italy who were discharged from the hospital after recovering from COVID-19.
The assessment found that 87% of the patients experienced one or more COVID-19 symptoms an average of 60.3 days after the onset of their first symptoms, with 55% of patients reported experiencing three or more symptoms. Among the most common symptoms experienced were fatigue, shortness of breath, joint pain and chest pain.
It is not known whether or not fully vaccinated people who still contract COVID have lower rates of long COVID, McLaughlin said during the press briefing, noting that the abstract nature of the condition means it is not a “reportable” condition in Alaska or in any other state.
State Pharmacist Dr. Coleman Cutchins during the press briefing also emphasized the role of vaccines in combating viruses generally.
“We do see this post-acute syndrome in other viruses, most notably mono(nucleosis), and there really isn’t any treatment option for it and there really isn’t even a clear understanding of the pathogenic process that makes it happen. It’s pretty much supportive care,” Cutchins said during the press conference. “So I think … get the vaccine and make yourself less likely to get this is really the only other treatment option. … Vaccine is how we treat viruses.”
Central Peninsula Hospital External Affairs Director Bruce Richards said that the CPH has seen some patients visit their primary care physician for lingering COVID-19 symptoms, but that incidents of long COVID are not something the hospital is tracking.
“I am sure (cases) are out there; we just haven’t been informed about any of them,” Richards said, adding that that could be due to individuals not seeking care for lingering symptoms or because they are seeing non-CPH providers.
The U.S. Centers for Disease Control and Prevention announced Monday that a “real world” study of mRNA vaccine efficacy affirmed that they are highly effective in preventing COVID-19 infection. The study was conducted among 3,950 essential and front-line workers, including health care personnel and first responders, and found that the effectiveness of full immunization was 90% against COVID infections regardless of symptom status. Effectiveness of partial immunization was 80%. Full immunization refers to individuals who are at least 14 days out from their second vaccine dose, while partial immunization refers to individuals who are at least 14 days out from the first dose but before their second dose.
Clinics geared specifically toward treating post-COVID symptoms have launched across the country, including in New York, California and Pennsylvania. The first and largest is at Mount Sinai in New York City, which launched the Center for Post-COVID Care last May.
“Although many patients with the virus experience upper airway and respiratory symptoms in the acute setting, mounting evidence suggests that these patients are also at risk for multiple systemic complications including thromboembolic disease, systemic inflammatory response syndrome, cardiovascular complications, and hepatic and renal impairment,” said a Mount Sinai press release announcing the center.
The push for greater vaccination efforts by Alaska’s public health officials comes as about 28% of eligible Alaskans have been vaccinated in the state and as more contagious COVID variants emerge around the world. To date, the state has identified 53 cases of COVID-19 variants of concern and variants of interest. Forty three of those are the B.1.429 variant, which was first detected in California.
State and local health officials have consistently emphasized the benefits of getting vaccinated. In addition to being highly effective at preventing COVID-19 disease, vaccines provide more robust immunity than natural infection. It is also free to receive the vaccine, while it is not free to be hospitalized with COVID.
Andrea Hooper, a nurse with the Kenai Public Health Center, noted that the average cost of a hospital stay in the United States is about $10,000 and can be higher in Alaska. Additionally, the average cost of an ICU stay in the United States is about $40,000. Hospitalizations and deaths are low among people who are vaccinated, Hooper said, and pose little risk of side effects. For every million people who are vaccinated, there are about 4.7 cases of serious anaphylaxis.
The CDC also recently said that people who are fully vaccinated can visit with other fully vaccinated people indoors without masks or social distancing, visit with unvaccinated people from a single household if low risk and with no masks or distancing and do not have to quarantine after exposure to a known case of COVID-19.
People who would like assistance with scheduling an appointment to be vaccinated can call the Kenai Peninsula Borough Office of Emergency Management call center. The center operates Monday through Friday from 9 a.m. to 12 p.m. The central peninsula call center can be reached at 907-262-4636. The Homer call center can be reached at 907-235-4636. The Seward call center can be reached at 907-224-4636.
A map of vaccine providers can be found on DHSS’ COVID-19 vaccine website at covidvax.alaska.gov. Many providers are using the state’s program to schedule appointments, which can be accessed at myhealth.alaska.gov. Instructions on how to schedule an appointment with a provider that does not use the state’s scheduling system can be found on the provider map by clicking on the icon of the provider through which people would like to schedule an appointment. Appointments at Walmart can be scheduled at walmart.com/covidvaccine.
More information about COVID-19 in Alaska can be found at dhss.alaska.gov.
Reach reporter Ashlyn O’Hara at ashlyn.ohara@peninsulaclarion.com.