Capacity expands at South Peninsula Hospital while Homer Public Health tracks down case contacts
Published 1:30 am Wednesday, April 1, 2020



With two Homer residents confirmed to have COVID-19, the disease caused by the novel coronavirus SARS-Cov-2, South Peninsula Hospital staff and public health nurses are putting boots to the ground to get Homer’s health care sector prepared and to protect its residents.
From reconfiguring windows in patient rooms to making more negative pressure rooms for potential patients with COVID-19, to creating an entire alternate care site with beds at Christian Community Church, the hospital is preparing for a likely increase in patients due to the steadily rising numbers of COVID-19 cases in the state. Meanwhile, members of the Homer Public Health team are tracking down potential contacts between the two Homer residents who have tested positive and others they could have encountered.
South Peninsula Hospital reported its first confirmed COVID-19 case within the Homer area on Saturday, March 28. The person was tested at the local hospital earlier that week, according to a press release from the City of Homer Unified Command. The person’s test was conducted by the Alaska State Public Health Laboratory.
This was the second COVID-19 case to involve a resident of Homer, but the first one to occur actually within the city. The first case was that of a Homer resident who was returning from traveling outside the state. The person was tested when they landed in Anchorage, and remained in Anchorage for isolation.
HOW DOES CASE INVESTIGATION WORK?
Nurses with Homer Public Health are tasked with conducting case investigations and tracing contacts the two confirmed COVID-19 patients may have had with others in the community. As Public Health Nurse Lorne Carroll explains, certain responsibilities for public health rest on the state, according to the Alaska Constitution and supporting state statutes.
This is important when it comes to “conditions reportable,” which Carroll explained are communicable diseases, like the novel coronavirus. As it stands, the state’s health care system allows providers to be reimbursed for services through coding. There’s a code for getting a flu shot, a code for a visit to the emergency room — but no code that allows health care workers to be reimbursed for disease investigations and interventions. That’s why it’s important that the state offers those services, Carroll said.
In Homer, a public health nurse staff of three is currently investigating cases of COVID-19 and doing contact tracing, or tracking down the potential contacts between those who have tested positive and those around them.
“The public health nurses are really good at it because they have experience with (investigating) sexually transmitted diseases,” Carroll said.
When it comes to these conditions reportable, which includes diseases like COVID-19 caused by novel viruses, Carroll said state statutes mandate that any time a health care provider or a lab feels they have a case on the conditions reportable list, they have to report it to the state. That report gets sent to the Department of Health and Social Services Section of Epidemiology. From there, the Section of Epidemiology would in turn notify the public health nurses in the community where the case originated, so that they could begin their investigations.
The unique thing about Homer, Carroll said, is that the local medical centers and primary care providers take it upon themselves to report cases not only to the state, but to Homer Public Health as well, in order to expedite the process.
Once a report of a case gets to the public health nurses, their official investigations can begin. Often, those case reports will include limited information like the person’s name, their date of birth, and the fact that they tested positive for a disease or virus.
“The public health nurse needs to do a full investigation surrounding that person,” Carroll said.
Usually, the patient’s primary care provider has already notified them that they have tested positive for whatever the disease or virus is. A public health nurse starts with a confidential initial interview, one which Carroll said can last up to 60-90 minutes. In that initial interview, the nurse is looking for information like whether the person traveled recently, where they traveled and under what conditions they traveled, as well as their recent social history. The public health nurse will ask for household contacts and any people that the patient is usually close to.
What the public health nurse is looking for in particular are “significant contacts.”
“A significant contact is defined as someone who’s been within six feet of someone with a lab confirmed (case of) COVID-19, and 10 minutes or longer,” Carroll said.
The public health nurse makes a list of all high-priority contacts, and contacts all of them directly, he said. Nurses will check up on these people to see whether they are experiencing any signs or symptoms of illness, and also to give them instructions on how to self quarantine for 14 days. If one of the significant contacts does report having symptoms, the public health nurse will give them instructions on how to immediately self isolate, Carroll said.
The next step is for that person to contact their primary care provider for further instructions and potential testing.
The number of people public health nurses have to get in touch with when tracing significant contacts varies greatly from case to case, Carroll said. However, he reported that with the two Homer resident cases of COVID-19 so far, those lists have been very short.
“And it’s because the (people) that we’ve talked to in the cases so far were already hunkering down at the times that they starting showing symptoms,” he said.
People can be infected before they start showing any symptoms of COVID-19.
“But if you’re … hunkering down at home, that makes it very easy for us because there’s not as many people to contact, and also it means there’s not as many people getting infected.”
Carroll also noted that, compared to other Alaska communities, Homer is doing well when it comes to following the state mandates and Centers for Disease Control recommendations for self distancing and staying at home. He knows this because, with only about 158 public health nurses statewide, the Homer public health nurses have been helping out and covering cases for other parts of the state.
“It really shows through these confidential case interviews and contact tracing,” Carroll said.
With COVID-19 confirmed for two Homer residents and one case confirmed within the community, residents might be concerned about whether they could have been in close contact with either case while out and about in town. For example, what if you were in the grocery store at the same time as a person with COVID-19?
Carroll explained that the novel coronavirus is not airborne, but rather is passed through respiratory droplets. These droplets would be spread to others when the person sneezed or coughed, he said. But the droplets drop out of the air after about 4-6 feet, finding something to land on. That’s why the recommended distance to stay away from other people is 6 feet. Beyond that distance, the respiratory droplets do not continue moving through the air.
Respiratory droplets can settle on surfaces, so Carroll emphasized the importance of constant hand washing and avoiding touching one’s eyes, nose or mouth.
Additionally, Carroll encouraged people to stay healthy, stay connected with others even while social distancing, and to get outdoors when possible.
PREPARING FOR PATIENTS
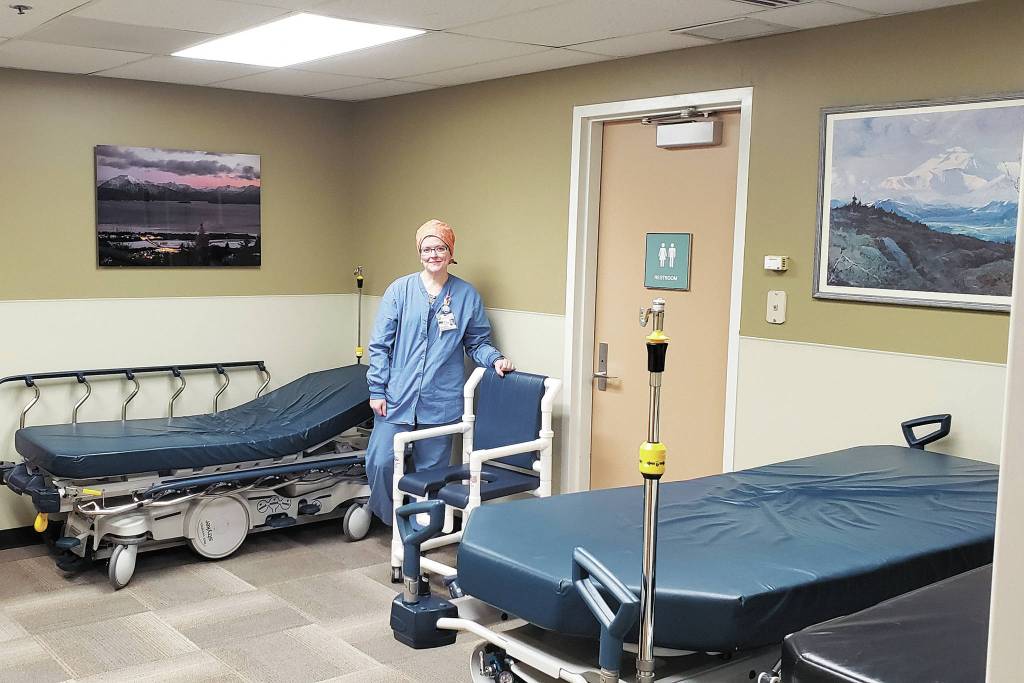
As public health nurses investigate the two known COVID-19 cases associated with Homer residents, South Peninsula Hospital is preparing for the onset of many more. Public Information Officer Derotha Ferraro detailed big changes at the hospital to create space and caring capacity for future COVID-19 patients, as well as maintaining space for those with other medical needs, like regular appointments or emergency care.
As of Wednesday morning, the hospital has collected 60 samples and sent them off for testing, with 39 of those tests coming back negative. The hospital has had one test come back positive so far, so the other 20 are still pending.
No patients with COVID-19 are currently being hospitalized in Homer, but the hospital is preparing for when that does start happening. All patients with COVID-19 will be completely separated from patients who are at the hospital for other reasons. What is normally the hospital’s inpatient unit has been transformed into an area specifically for patients with COVID-19. There are normally 18 beds in this section of the hospital, but by moving furniture and adding a second bed to some rooms, Ferraro said that capacity has been raised to 30 beds.
Before now, South Peninsula Hospital had two isolation rooms, or negative pressure rooms, in the inpatient unit. These are rooms where air is circulated in a way that it does not connect to other rooms in other areas of the hospital, thus keeping other patients from getting infected. Lakeshore Glass was slated to arrive at the hospital on Wednesday to remove side panel windows from some of the inpatient rooms that have been designated for COVID-19 patients. From there, crews will reconfigure the air flow of those rooms to turn them into isolation rooms.
In addition to the 3o beds in what used to be the inpatient unit, the hospital has created an alternate care site for future COVID-19 patients at Christian Community Church, just a few blocks down Bartlett Street from the hospital. There are enough beds, supplies and equipment there to care for 40 COVID-19 patients, Ferraro said, but the church building has the floor space to house more than 100 patients safely. The hospital has submitted a request to the state to get more beds and equipment, Ferraro said.
Since the hospital’s inpatient unit has been transformed into a place for COVID-19 patients, the hospital has found other places to care for people who have other needs, such as emergency care or childbirth. The surgery department and the physical therapy department have both been turned into places for regular inpatient care. Those needing care not related to COVID-19 will come through the main hospital entrance and proceed to whatever department they need, such as the birthing wing or toward the inpatient beds in the surgery department or physical therapy department.
Physical therapy services have been moved to the hospital’s specialty clinic, and infusion services are now being offered out of the Behavioral Health building.
Additionally, Ferraro said Homer Medical Center will be open every day until 8 p.m. and will supplement care for less serious emergencies. People with a medical emergency should come to the emergency room in the hospital, but should be aware that they may be sent to Homer Medical Center for care.
All of these alterations and creating more capacity to house patients is part of how South Peninsula Hospital is following state guidelines on how COVID-19 patients will be treated according to their symptoms.
“The COVID patients will be separated into what they’re calling mild, moderate, urgent and severe (categories),” Ferraro said.
Those with mild symptoms will be sent home to self isolate until they recover. Then there are those with moderate symptoms.
“Those are patients, based on the conditions they’re experiencing, who will recover easily just with a minimal amount of hospitalization care,” Ferraro said.
It’s those moderate patients who will go to the alternate care site at Christian Community Church. Patients categorized as urgent will receive care in the transformed inpatient unit, which is now sealed off at both ends to keep it separate from other areas of the hospital.
Ferraro said, depending on how many patients are in the hospital at once, South Peninsula Hospital does have the ability to care for patients categorized as severe. However, the other option is to have those patients flown to designated COVID-19 hospitals in Anchorage.
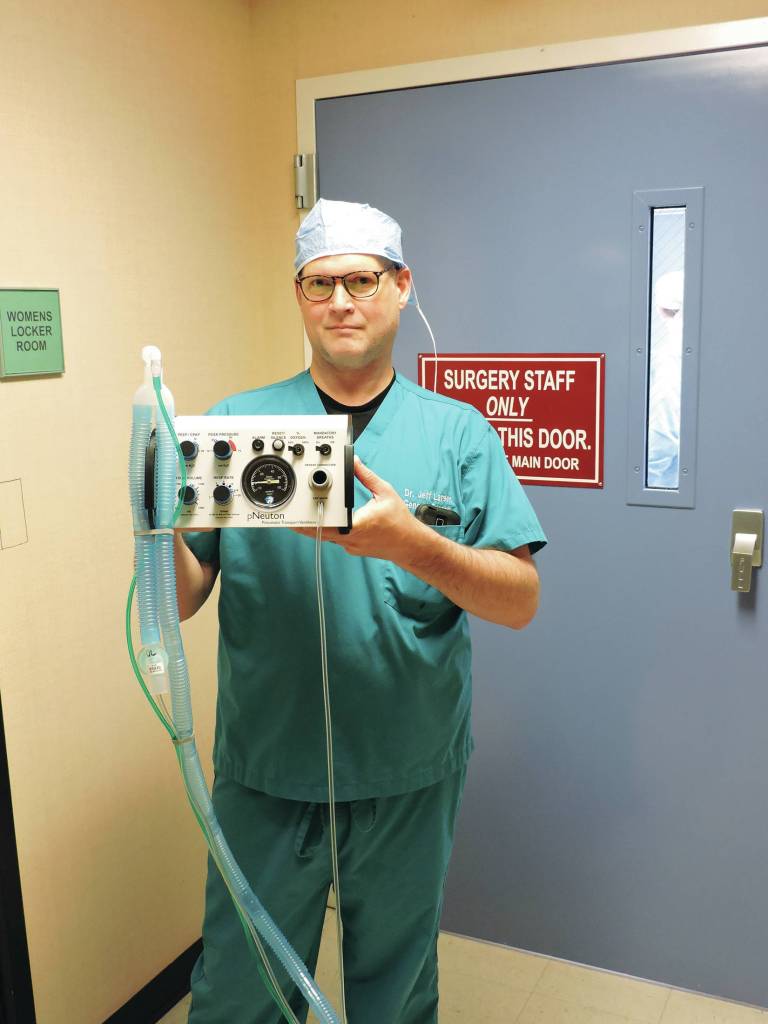
South Peninsula Hospital now has nine ventilators, which are needed by COVID-19 patients who have trouble breathing. There were already three in the acute care unit, Ferraro said. There were another three in the surgery department for anesthesia which have been repurposed, as well as one that had previously been designated for transport. That particular ventilator is safe to use in an MRI machine, so patients can take it with them if they need a scan, Ferraro said.
An additional two ventilators have been given to the hospital by local emergency medical technicians.
Staff at South Peninsula Hospital have been busy learning about the virus, and becoming familiar with the protocols for treating patients and staying safe and clean while doing so, Ferraro said. The hospital is currently in need of the following items if people are looking for things to donate:
• Gloves (size small, medium, large and XL)
• Unopened hand sanitizer
• Procedure/surgical masks
• Hand-sewn hair/head covers
• Hand-sewn face masks
• Disposable gowns or coveralls
Items cannot be donated directly to the hospital. Do not take items to the hospital campus. All donations are currently being routed through the City of Homer, which will distribute them to the appropriate places. To donate, complete the donation form on the city website at https://www.cityofhomer-ak.gov/covid19/donations-volunteering.
Ferraro stressed that the staff at South Peninsula Hospital is still seeing people who aren’t following the state mandates and recommendations from the CDC.
“If people would just follow those recommendations, it would honestly save lives,” she said. “And that’s the biggest, most important request from our medical staff, is to distance yourself and follow these recommendations.”
The Homer Public Health Center is offering flu shots free of charge. Getting a flu shot will not protect you against the novel coronavirus, but will protect you against the flu this season. This, in turn, will reduce the number of people needing to go to the hospital to be treated for the flu. That frees up vital beds and space, Carroll said.
“I like to think of it as, we’re gearing up and planning for the worst case scenario, and I don’t know that that’s going to happen, but we want to preserve precious health care resources for those who may need it in the future,” he said.
Call 907-235-8857 for a free flu shot. Ferraro emphasized the importance of calling ahead for all medical appointments, and even emergency visits to the hospital. Medical staff encourage calling before you come or calling from your vehicle once you arrive.
Reach Megan Pacer at mpacer@homernews.com.