At a distance of 220 miles and a 40-minute flight from South Peninsula Hospital to Anchorage, the time and distance can present challenges for getting intensive care at the lower Kenai Peninsula’s only rural hospital. If the weather is bad, LifeMed and other medevac services can’t fly. Patients might also prefer to say in Homer, where they can be close to family and friends.
In rural emergency service areas like Anchor Point Emergency Services and Kachemak Emergency Services, medics face a similar challenge. KES responds from Diamond Ridge to Kachemak Selo, and with rides sometimes taking a half-hour or longer to get to the hospital, getting not just emergency response but information between medics and emergency room staff can be critical in saving lives.
New advances and equipment in telemedicine by emergency services and South Peninsula Hospital are helping to bridge the gap. Among the technologies and programs now being used are:
• The Phillips MRX telemedicine unit that transmits by cell-phone signal vital information like heart rate, blood pressure and oxygen levels from an ambulance to South Peninsula Hospital as the patient is on the way;
• eICU, A 24-hour, seven days a week contract between SPH and Providence Alaska Medical Center, Anchorage, where critical care nurses and doctors in Anchorage can provide immediate advice to the SPH emergency room, and
• An eICU — electronic Intensive Care Unit — machine with two-way video conferencing that also can transmit vital information from Homer to Anchorage.
“Telemedicine is just exploding. Homer is an amazing place to work with our team,” said Sharon Compton, a critical-care registered nurse and clinical services manager for eICU at Providence.
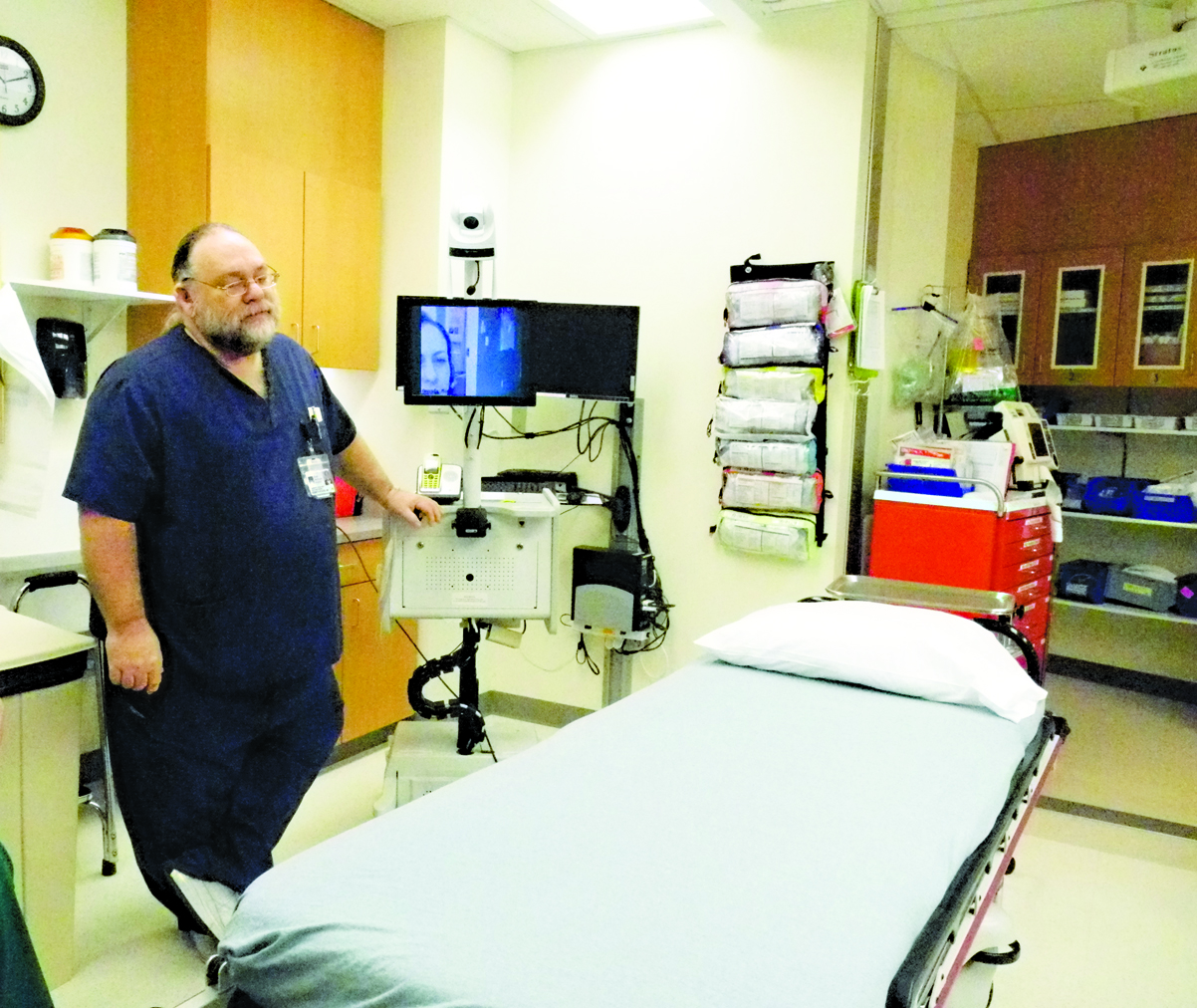
Earlier this month, Compton was in Homer to train local medical staff in using the eICU system. Central to that system is a battery powered telepresence unit that can be moved on wheels in the ER or to patient beds. The unit has a video screen that shows the face of the on-call critical care nurse at Providence. The Providence nurse can rotate 180 degrees a camera on the eICU unit to look at the patient and check for things like dilated eyes.
If someone in the ER needs advice from Providence, “In real time, at a push of the button, I can have someone here,” said Kenny Rogers, director of the SPH emergency department.
“It’s an extra set of eyes and ears,” Compton said.
Providence also can get real-time information transmitted from the ER. The numbers and wiggling lines patients see on monitors on the machine by their beds also get sent up to the eICU staff.
Except for the visual connection, the information being sent from SPH to Providence also can be sent from an ambulance on its way to the hospital to the ER.
“We’re doing with emergency medical services what Providence is doing with eICU,” Rogers said.
Every KES ambulance has an MRX unit, paid for by a Code Blue grant from the state of Alaska, a program that provides financial support to rural health services, said KES Chief Bob Cicciarella. When a medic responds, electrocardiogram information and other vital signs gets connected to the MRX.
“By pressing a button on the monitor, the medics can then begin live transmission to the emergency techs at SPH,” said KES Assistant Chief Steve Boyle.
Medics also are in radio contact with the hospital, but the MRX frees them up from having to make frequent radio calls in with that information. The ER team also can see analog information like wave forms — the wiggly lines on a heart monitor.
“The kind of cool thing about this is it lets us work at a paramedical level and have the physicians up to speed without me having to stop what I’m doing,” Boyle said.
He cited a recent call where a patient had an aortic aneurysm — a bulge in the wall of an artery feeding the aorta of the heart. The ER got critical information and could start making preparations like having the patient taken directly to get a computerized tomography, or CT, scan. The ER doctors also put a fixed-wing medevac plane on alert ready to come to Homer.
“When we hit the ER, the doctor was up to speed,” Boyle said. “It certainly made a difference.”
At the hospital, eICU also can be used outside of the ER. The eICU unit can be wheeled to a patient’s bedside, with a nurse at Providence monitoring the patient remotely. That might mean a patient doesn’t have to go to Anchorage.
“If you keep a patient in their home (town), with the transport fee the family dynamics — it pays for itself,” Compton said.
Rogers said patients have to be informed about the unit so they won’t be alarmed to suddenly see the image of a person on the screen and the camera looking at them. Cameras are turned away when not being used to protect patient privacy.
Providence even uses eICU in its own critical care units, with eICU staff monitoring patients.
“eICU supplements the on-floor nurse,” Compton said. “It doesn’t take away the physician from the patient.”
SPH funds the eICU program out of its operating budget, said Shara Sutherlin, director of SPH patient services.
Telemedicine has lead to another change in medicine. Turf wars between physicians, ER nurses and critical care nurses are becoming the thing of the past, with specialists now collaborating more with others.
“Health care is a team sport. To do things like this, you have to learn more. Everybody gets smarter together,” Sutherlin said.
“Telehealth is really the up-and-coming,” Compton said. “If you can think it, you can do it.”
Michael Armstrong can be reached at michael.armstrong@homernews.com.